This post examines mental health in tech and which workplace policies are most associated with higher treatment-seeking among employees.
TL;DR
When it comes to mental health, tech workers report a big trust gap: they expect negative consequences for discussing mental health far more than physical health. As a result, they don’t even look into what the policy at their company is. That is a major problem because awareness is as critical as access. Across benefits, care options, resources, anonymity, and wellness talks, “Don’t know” responses track almost as poorly as “No.”
A higher support score (visible benefits + clear options + resources + anonymity + wellness dialogue) is strongly associated with treatment-seeking, with big gains up to ~3 policies understood/visible.
The business case is real: new research estimates burnout costs U.S. employers $4,000–$21,000 per employee per year(≈ $5M/yr for a 1,000-employee firm). Meanwhile, ~40%+ of tech workers have a high risk of burnout.
The tech industry runs on attention and problem-solving—exactly what chronic stress erodes. I analyzed the Open Sourcing Mental Illness (OSMI) Tech Survey to quantify how visible, trustworthy workplace policies relate to help-seeking for mental health. The goal: turn anecdotes into actionable, ROI-aware guidance for teams and leaders.
Data & Method (quick tour)
- Dataset: OSMI Mental Health in Tech Survey (2014), 1,259 respondents, 27 variables (e.g., demographics; workplace policies: benefits, care options, wellness talks; perceived anonymity; and outcomes like treatment-seeking, work interference).
- Key construct — Support Score: For each policy question, Yes = 1; No/Don’t know/Not sure = 0; sum across items → per-person support score.
- Stats: Welch one-way ANOVA + pairwise Welch t-tests to compare treatment-seeking across policy categories and risk factors (age, gender, family history, work interference).
What I found
- Big stigma & trust gap
Employees fear negative consequences far more when discussing mental vs physical health with employers. That effectively suppresses early help-seeking and exacerbates presenteeism.
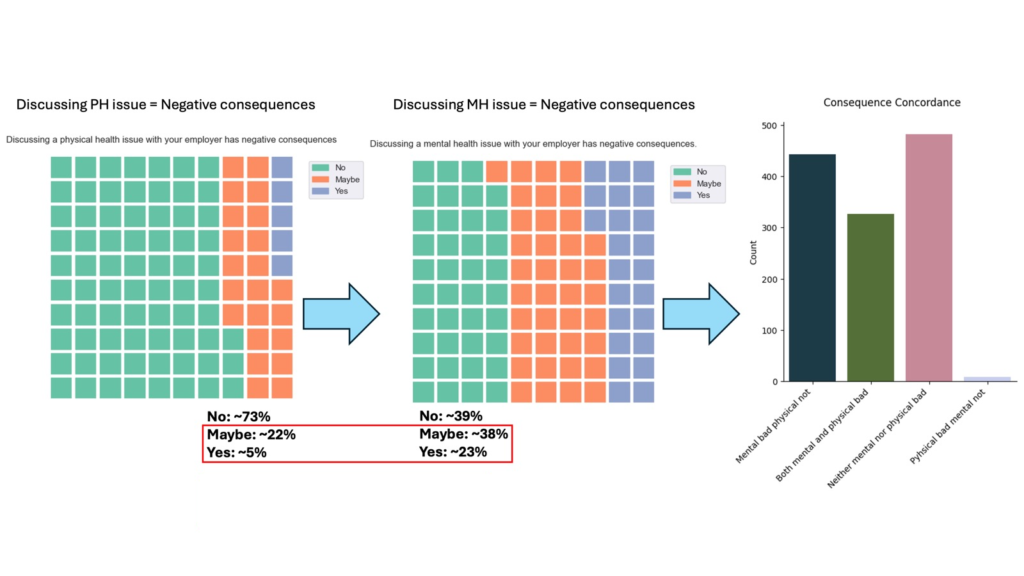
(PH: Physical Health; MH: Mental Health)
- Awareness is leverage (and often missing)
For benefits, care options, resources, anonymity, and wellness programs, large shares answered “No” or “Don’t know.” Those “Don’t know” groups repeatedly underperform “Yes”—often similar to “No.” In other words: communication gaps erase ROI.
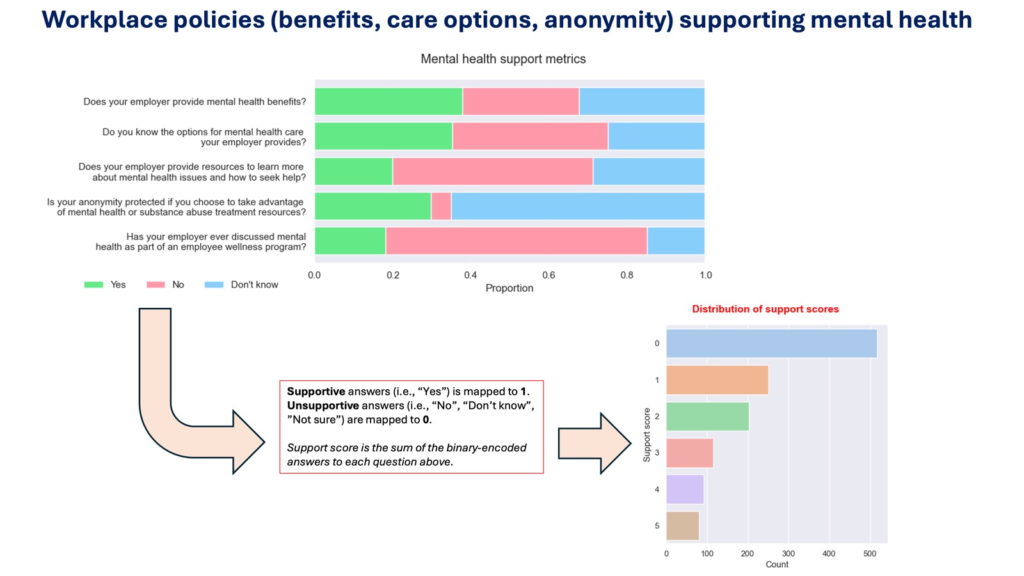
- Support drives action
Higher support scores correlate with higher treatment-seeking, with strong gains up to ~3 understood/visible policies (then a plateau). Practical takeaway: while you may not need every program, it is critical to make a few core policies visible and trusted.
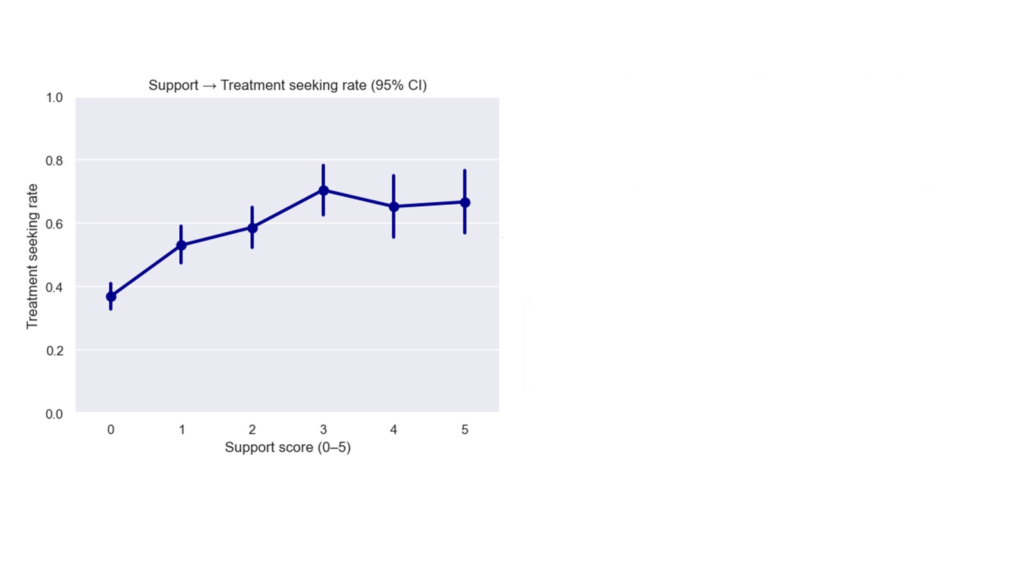
One-way ANOVA followed by pairwise Welch’s t-test:
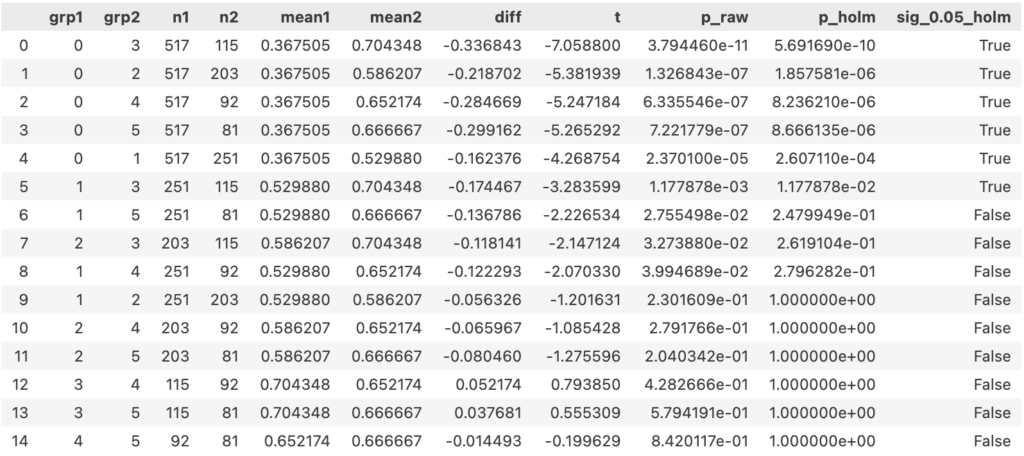
Employees with support score ≥1 were more likely to seek mental health treatment than those with support score 0.
- Benefits present → higher treatment-seeking. Lack of awareness can be worse than not having benefits.
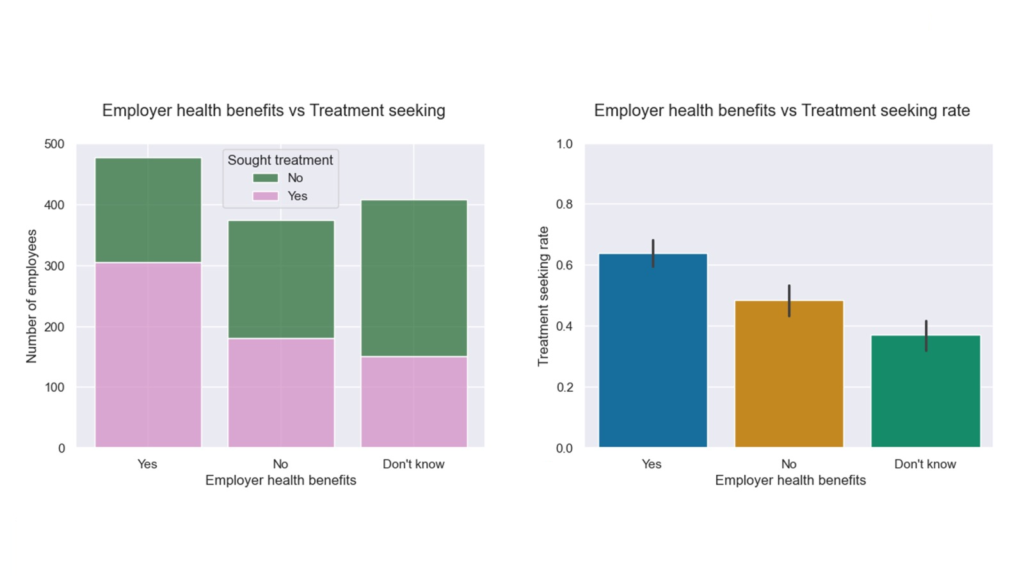
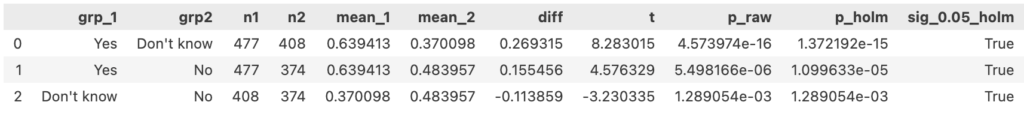
One-way ANOVA followed by pairwise Welch’s t-test:
- Know your options → action spikes. When employees know what care options are available to them, they’re far more likely to seek help.
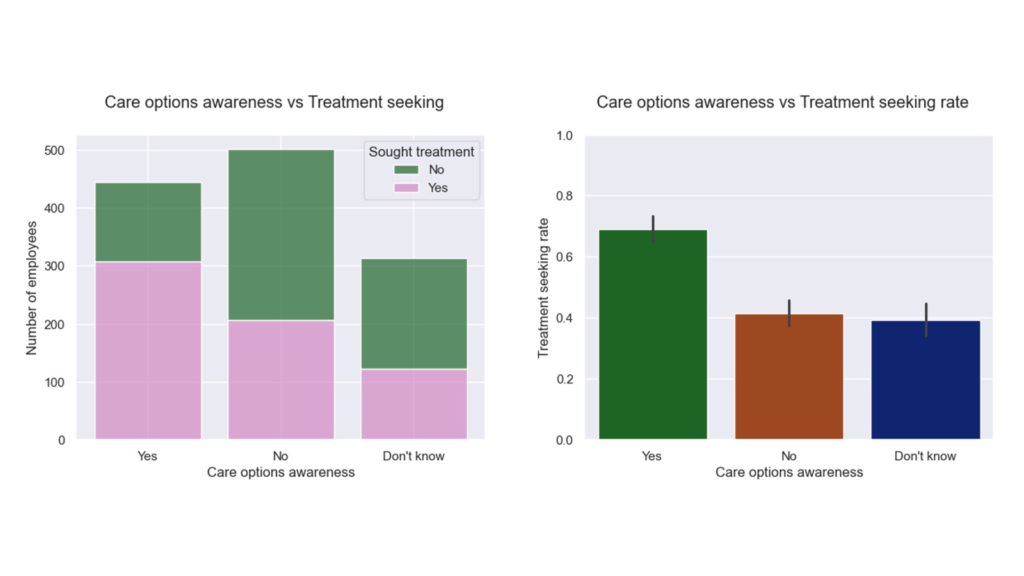
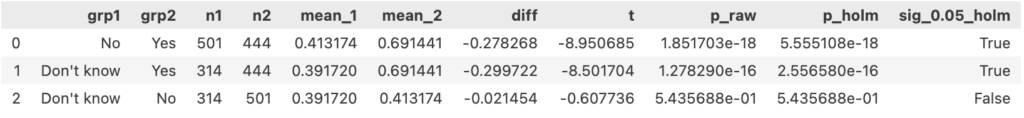
One-way ANOVA followed by pairwise Welch’s t-test:
- Resources provided → highest treatment-seeking (~59%). Practical guides matter.
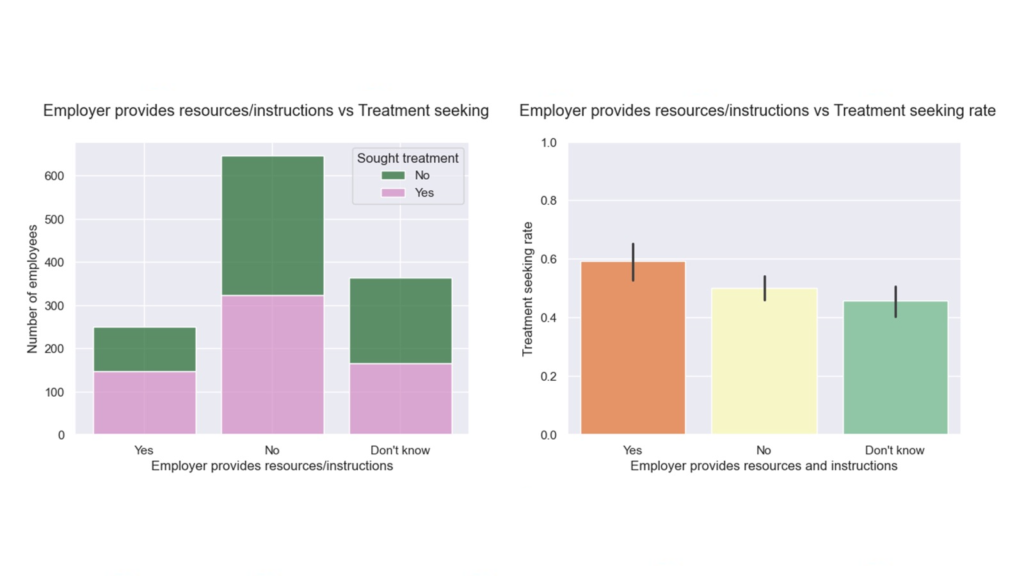
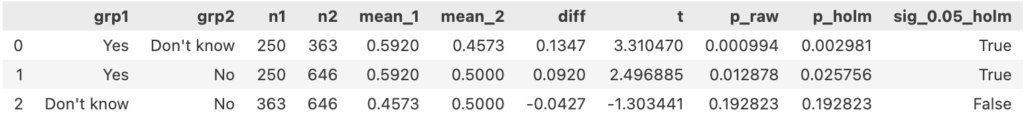
One-way ANOVA followed by pairwise Welch’s t-test:
- Wellness talks → higher help-seeking. Silence signals risk; conversation signals safety.
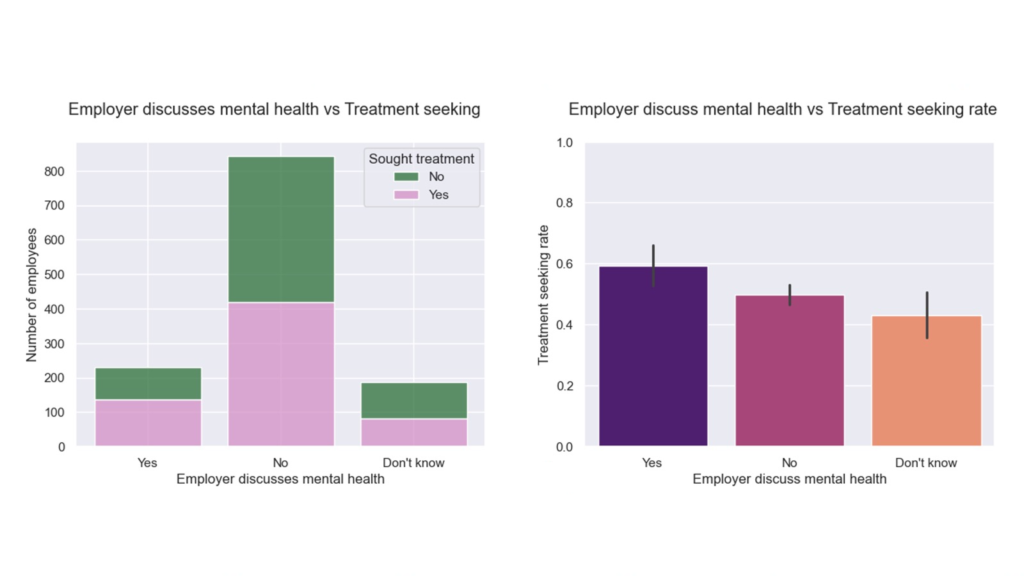
One-way ANOVA followed by pairwise Welch’s t-test:
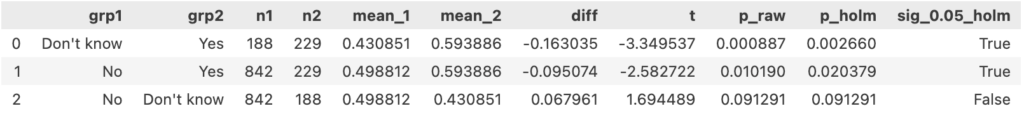
- Anonymity clarity beats ambiguity. “Not sure if I’m protected” depresses help-seeking more than a clear “No.”
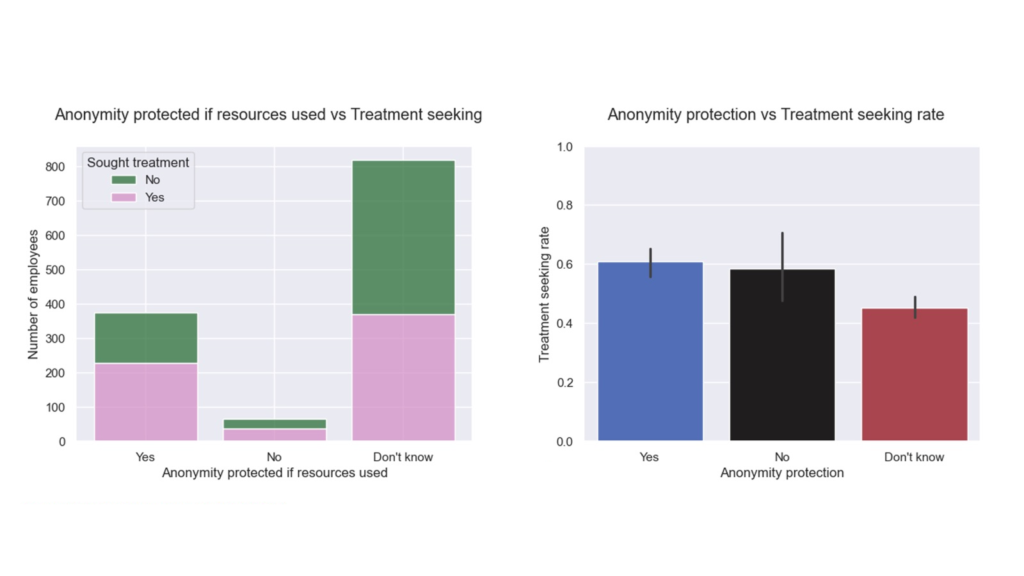
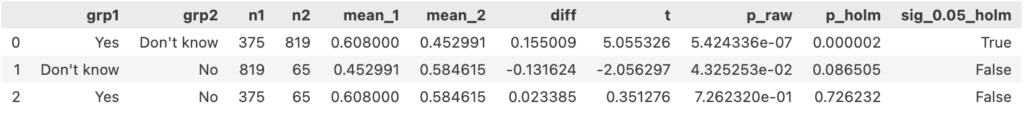
One-way ANOVA followed by pairwise Welch’s t-test:
- Who’s at risk?
- Younger men (<25 and 25–34) were least likely to seek treatment. Rates among men improve after 45, approaching women’s rates. Targeted manager training and tailored messaging can help ameliorate the age and gender gap.
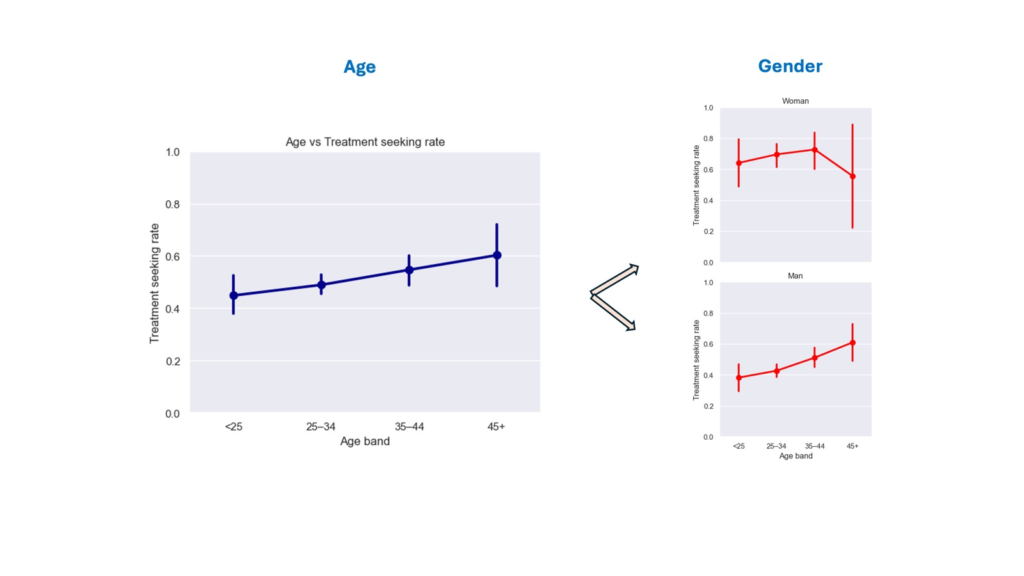
One-way ANOVA:

Age-group differences in treatment-seeking did not reach conventional statistical significance (Welch one-way ANOVA, p = 0.058), but the near-threshold p-value provides weak evidence consistent with a small age effect in this sample.
- Family history of mental illness is linked to higher treatment-seeking—likely via awareness and recognition.
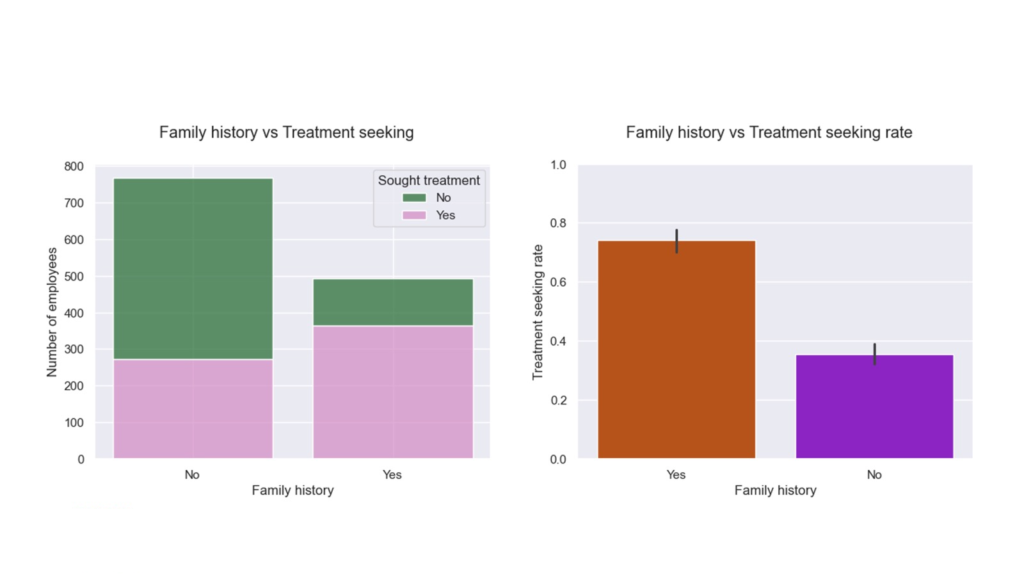
Welch’s t-test:

- Work interference is a strong signal of demand. Those reporting frequent interference seek care much more often(significant Welch tests). Capacity planning should account for this.
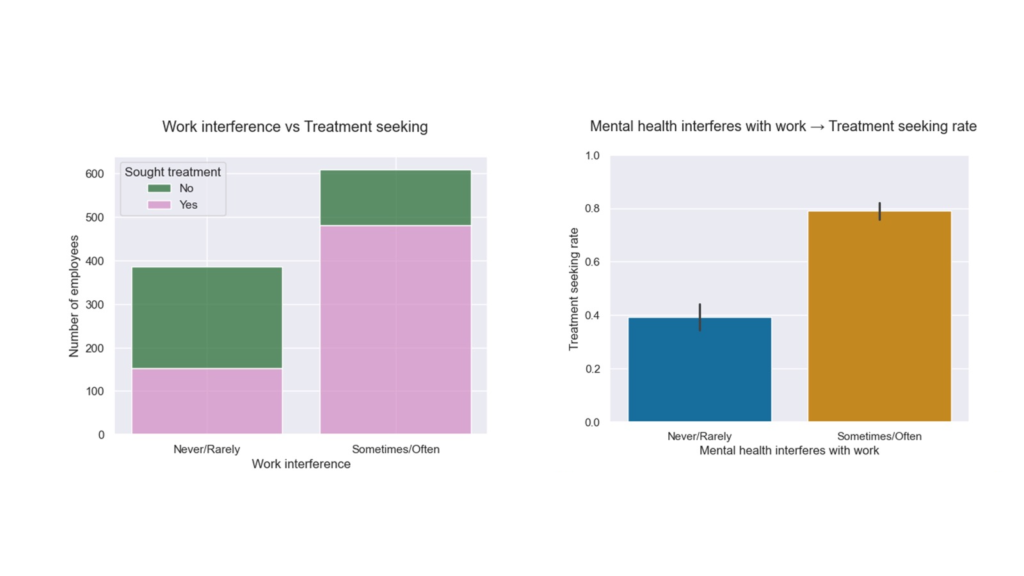
Welch’s t-test:

Why this matters (for teams & CFOs)
- Human lens: The Yerbo Burnout Index reported ~42% of tech employees at high risk of burnout,a problem that predates and outlasts any hype cycle.
- Business lens: A 2025 American Journal of Preventive Medicine study estimates $4,000–$21,000 per employee per year in burnout costs, indicating a significant loss of ~$5M/yr for a 1,000-person company. That’s real money you can reinvest in policy visibility, manager training, and privacy-preserving access to care.
4 recommendations for tech business leaders
- Make 3 policies unmistakably visible. Prioritize benefits, how-to-access care, and anonymity protections. Repeat the message in onboarding, manager 1:1s, and quarterly refreshers.
- Train managers for safety signals. Equip them to open conversations without prying; normalize early help-seeking; route to resources.
- Measure trust, not just availability. Track “Don’t know” rates and anonymity confidence; treat them as leading indicators.
- Plan capacity where interference is high. Where work interference is common, expect higher demand for counseling/EAP and adjust bandwidth accordingly.
Limitations & future work
- Single-year, self-reported data (2014): The data is representative of its sample/time; not a full longitudinal view. Extending to later OSMI waves can validate trend stability and expand subgroup analysis.
- Associational (not causal): Strong correlations guide where to experiment; organizations should A/B their policy visibility and communication strategies to test causal lift.
References
- State of Burnout in Tech (2022, Yerbo): Estimates ~42% of tech employees at high risk of burnout.
- American Journal of Preventive Medicine (2025): “The Health and Economic Burden of Employee Burnout to U.S. Employers” — estimates $4,000–$21,000 per employee per year; ≈ $5M/yr for a 1,000-employee firm.
Footnotes
This post summarizes the methods, figures, and results presented in my talk, “Mind Over Machines: Exploring Mental Health in Tech Workers — Exploratory Data Analysis with Python.”

Leave a Reply